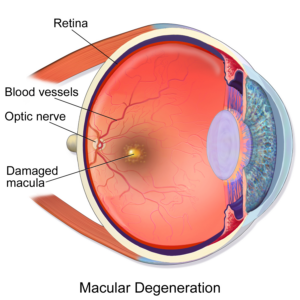
 Macular degeneration (also known as Age-Related Macular Degeneration, ARMD or AMD) is the most common cause of severe, central vision loss among Americans over 50 years old. Macular degeneration is a condition in which the macula deteriorates over time. The macula is the center of the retina which is responsible for our ability to discern fine detail, necessary for visual tasks like reading and recognizing faces. Ophthalmologists refer to this as central vision.
Macular degeneration (also known as Age-Related Macular Degeneration, ARMD or AMD) is the most common cause of severe, central vision loss among Americans over 50 years old. Macular degeneration is a condition in which the macula deteriorates over time. The macula is the center of the retina which is responsible for our ability to discern fine detail, necessary for visual tasks like reading and recognizing faces. Ophthalmologists refer to this as central vision.
Very early stages of macular degeneration may not affect the vision at all. Other cases, unfortunately, can cause a large central blind spot, and an inability to see faces or read. The goal of regular retina exams and home monitoring is to catch deterioration early, in hopes that it can be treated and save as much central vision as possible.
The two types of AMD are commonly referred to as dry macular degeneration and wet macular degeneration.
Dry macular degeneration is the more common of the two types of macular degeneration, affecting over 80% of people who have Age-Related Macular Degeneration. Vision deterioration in dry AMD occurs more slowly than in wet AMD. Since wet AMD refers to bleeding or fluid in the macula, dry AMD is used to describe macular degeneration in which there is no bleeding or fluid. This typically involves small, yellow deposits under the macula, called drusen, and/or changes to the pigmented cells under the macula, called retinal pigment epithelium. Typically little to no vision loss occurs until the middle and later stages of dry AMD, thus it is important to get regular eye exams to ensure that this condition is detected early. Additionally, there are certain indicators on your exam, like how much drusen is present, that can alert us if you are low or high risk for progression to wet AMD and vision loss. If you are moderate to high risk, we recommend AREDS 2 vitamins, home monitoring with an Amsler grid and more frequent follow-up exams.
Wet macular degeneration is a more advanced form of AMD. While accounting for under 20% of total cases of AMD, wet macular degeneration is responsible for over 90% of cases with severe vision loss. Wet Age-Related Macular Degeneration involves the growth of abnormal new blood vessels beneath the macula. These vessels often break and bleed, leaking blood and fluid which causes damage to the macula and rapid loss of eyesight. Patients who develop wet macular degeneration often develop sudden loss of central vision or central blind spot in one of their eyes.
The specific cause of macular degeneration is not known, but the disease tends to affect older people. Although it can affect people as young as 55 years old, it more commonly affects people in their 60s, 70s and above. Lifestyle factors also apply – smoking cigarettes has been shown to double the risk of macular degeneration. Obesity and cardiovascular diseases may also increase your risk. Race appears to be a factor as well, with most occurrences of AMD affecting people of Caucasian descent, although people of any race can be affected.
In the early stages of macular degeneration, it is quite common to have no apparent symptoms. Dry AMD may first manifest itself gradually as fuzzy, blurry or distorted vision, or seeing straight lines as wavy or curvy. Early symptoms in wet AMD often occur suddenly and may be a blurry or dark spot near the center of your vision.
If you do not have any symptoms, it is still important to get regular eye exams from a retinal specialist, as we may be able to identify drusen accumulation – an early indicator of dry macular degeneration – before any discernible effect on your vision has taken place. And if you do have any of the above symptoms, it is important to come in ASAP to determine if you have any new bleeding or fluid in your macula that may need urgent, sight saving treatment.
Macular degeneration is diagnosed by the presence of drusen, pigment changes, bleeding, and/or fluid in or under the macula. Some findings of dry AMD, such as drusen and pigment changes may be present before you have begun to notice symptoms. If there is bleeding and/or fluid in or under the macula, as in wet AMD, these findings are usually accompanied by vision loss, dark spot, blurry vision, or wavy lines.
If you are diagnosed with dry AMD, examinations every 3, 6 or 12 months are often recommended to monitor the progression of the AMD. For wet AMD, the doctor will likely recommend prompt treatment.

At home, self-monitoring can be performed using an Amsler grid. To use an Amsler grid, cover your right eye and look at the center dot with your left eye. Then cover your left eye and look at the center dot with your right eye. Do not scan around the grid with your eye. Focus only on the center dot while taking note of the surrounding intersecting lines. Any wavy lines or blind spots should be noted and reported to your retina specialist as they could be a sign of new bleeding and/or fluid under the retina and urgent sight-saving treatment might be indicated.
Wet macular degeneration cannot be prevented, therefore, the goal is to catch any possible progression to wet AMD early, which would allow for prompt sight-saving treatment. This is accomplished with routine, scheduled retina exams as well as self-monitoring at home with an Amsler grid in between appointments.
Fortunately, we have excellent treatments available for wet macular degeneration. Three main medications are used: Eylea, Lucentis and Avastin.
All three medications act to lower the amount of VEGF (vascular endothelial growth factor) in the eye. VEGF is a growth factor that causes new, abnormal blood vessel formation (neovascularization). These new blood vessels leak fluid and bleed under the macula, causing vision loss.
The medications are given through an injection into your eye during your office visit. Although this sounds very scary, we try to make the experience as comfortable as possible.
These are two of the most common questions we hear when discussing these treatments. Fortunately, the answer to both questions is no. You will not see the injection and you will not feel the injection. Your retina doctor and the team at NYC retina will work to customize a regimen for you that will eliminate all pain associated with the injection.
The way this works in most cases is: your retina specialist will instill eye drops to properly numb your eye and also drops to decrease the risk of infection. In some cases, a strong anesthetic will be administered under the conjunctiva (or skin of the eye) to further decrease any sensation associated with the injection. Then after a few minutes of allowing the numbing medication to work, you will either look down or look up, and the retina specialist will perform the injection. Because of the anesthetic that was placed, you will not feel the injection.
Additionally, depending on the severity of your macular degeneration, your retina specialist may recommend vitamins that may slow the progression of the AMD. The vitamins are called AREDS 2 which stands for Age-Related Eye Disease Study 2. AREDS2 is a combination of vitamin C, vitamin E, copper, lutein, zeaxanthin, and zinc. It is important for you to consult with your retina specialist to see if you are a candidate for these vitamins and then to coordinate with your primary doctor to make sure that there is no overlap with any of your other prescriptions or over the counter medications.
Research into the treatment of dry macular degeneration is ongoing. The doctors at NYC retina are committed to bringing you up to the moment information and treatments as they become available. As of now, however, there is no definitive treatment for dry AMD. Certain lifestyle changes may slow the progression of dry AMD. These include eating a healthy diet including green leafy vegetables, fish, omega-3 fatty acids (found in salmon and walnuts). Smoking cessation, when applicable, would not only decrease your chance of wet AMD and vision loss but also improve your overall health.
Additionally, the progression of dry macular degeneration to what is called geographic atrophy, with resultant central vision loss, has no treatment. However, although the pigment changes in dry macular degeneration cannot be reversed, we can often improve visual functioning by maximizing the condition of dry eye, cataracts, or glaucoma that may be present. In these cases, we will work with your general ophthalmologist or optometrist to help you achieve your best vision.
Finally, if you have AMD, you have received all treatments possible and you are still having trouble reading, you might need the help of low vision aids. Often, simply increasing the font on an iPad, tablet, or computer screen can make reading easier. You may discuss different options with your doctor.
Regular eye exams are essential for detecting macular degeneration early on in order to take steps to slow its progression (such as AREDS 2 vitamins) and possibly, prevent long-term vision loss. Additionally, during the exam, if there are any signs of wet macular degeneration your doctor will be able to treat you with potential sight-saving treatment.
Eating a healthy diet, as described above, may reduce your risk. Self-monitoring at home with an Amsler grid will help you catch any changes early and get prompt treatment. Finally, smoking cessation is critical not only to reduce your risk of wet AMD but also many other health issues.
If wet AMD is left untreated, it can cause permanent, central vision loss, severely impeding your ability to perform ordinary tasks like reading, driving and functioning independently.
Macular degeneration is a leading cause of central vision loss, especially in people 50 years old and older, affecting over 10 million Americans.
A healthy diet and lifestyle, AREDS 2 vitamins, and smoking cessation all help reduce the risk of progression from dry macular degeneration to wet macular degeneration.
Regular eye exams can detect any worsening that may need prompt, sight-saving treatment.
Prompt treatment of wet AMD with either eylea, lucentis or avastin increases the chances of maintaining central, reading vision.
Eye injections can be performed painlessly, in a comfortable setting by our team of experts at NYC Retina.
If you begin to notice blurriness, waviness, or a blind spot near the center of your field of vision, please schedule an appointment with one of our eye experts immediately.